Innovative Care Coordination System Saves Lives

As the woman struggled through the doors of the emergency department (ED) at UVM Health Network – Elizabethtown Community Hospital, Physician Assistant Alex Caffrey, knew she was looking at a person in desperate need of care. The patient was fighting to breathe, racked by asthma and a bout with COVID-19. The Ticonderoga campus is a state-of-the-art 24-hour emergency department and outpatient medical center, but Caffrey had a nagging feeling that this patient required more intensive care.
It was a complex situation and I knew I was going to need all of the resources at my disposal to care for this patient. I really wanted another set of eyes on her to gauge whether she needed to be transferred to another hospital for intensive care – and if so, to determine the safest way to do that.
Physician Assistant Alex Caffrey
Caffrey called the UVM Health Network Transfer Center and requested an emergency tele-video consultation, known as Tele-EM.
’There Is Nothing Better Than Getting Your Eyes on Them’
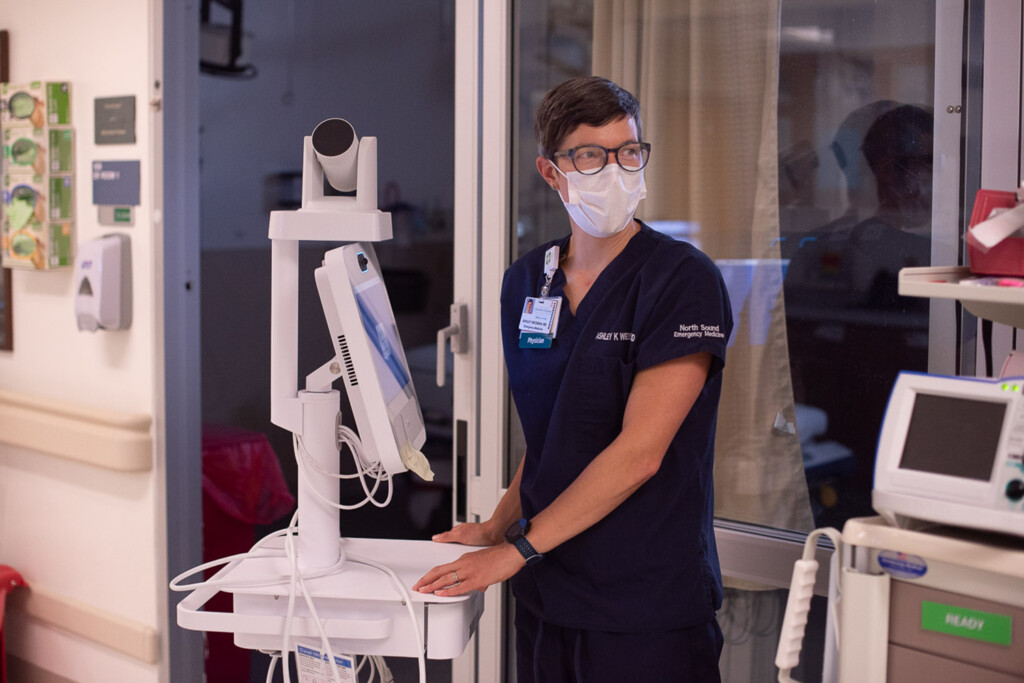
Ash Weisman, MD, was working in The University of Vermont Medical Center ED when she received the call. On the line was a nurse from the Transfer Center, who began briefing Dr. Weisman on the situation unfolding at Elizabethtown Community Hospital.
Despite being more than fifty miles away, Dr. Weisman was observing and evaluating the patient within minutes thanks to mobile telemedicine carts positioned at each hospital. Rolled out in recent years at all UVM Health Network affiliates, the carts help ED providers consult with each other via video on difficult cases or in emergency situations like a suspected stroke. And because the system is linked to the Network’s common electronic health record system, the carts also enable providers to share information and view and analyze in real time a patient’s blood work, tests or scans.
When you’re trying to make a tough call – like whether to intubate or transfer a critically ill person – there is nothing better than getting your eyes on them. In this case, our Tele-EM system made it easy for us to muster the expertise and resources we needed to get this patient the right care.
Dr. Weisman
The Care Coordination System
The ease with which Caffrey and Dr. Weisman connected is a testament to the strengths of the Transfer Center and its parent, the UVM Health Network Care Coordination System. Because much of this group’s work happens behind the scenes, its contributions are sometimes inconspicuous. When things go smoothly, its efforts fade into the background, leaving providers and nurses free to focus on providing fast, effective care.
Formed in 2017, the Care Coordination System brings together a collection of more than 130 health care providers, nurses, EMTs, paramedics and communications and logistics experts that work together to coordinate safe, seamless care for patients across Vermont and northern New York. The Care Coordination Systems provides the unsung services – like patient transfers, ambulance transportation and communication, or provider consultations – that connect the region’s hospitals (including those outside of the UVM Health Network) into a cohesive health system.
“Our goal is to quickly connect Network experts, technology and resources to provide high-quality care to every patient, wherever and whenever they need it,” says Ryan Clouser, DO, a critical care medicine physician and medical director of the Care Coordination System. “Ideally, we aim to get people that care close to home, but there are inevitably cases where we need to transfer people to give them the best chance of recovery.”
The Right Care at the Right Time
Back in Ticonderoga, Caffrey and Dr. Weisman’s collaboration was coming to this very conclusion. But Caffrey says that the logistics of such a transfer still presented cause for concern.
“We try to avoid intubating COVID-19 patients at all costs,” says Caffrey. “But there were real concerns that her breathing would give out during the one and a half hour ambulance ride to the UVM Medical Center. We needed a better option.”
Dr. Clouser joined the Tele-EM consultation that evening, offering remote triage from the Transfer Center, backed by his expertise as a physician in the intensive care unit at UVM Medical Center.
“Between the three of us, we agreed that while we didn’t need to intubate, the safest option was to airlift her to the UVM Medical Center for treatment in our ED,” says Dr. Clouser. “Our critical care transport teams are trained to deliver mobile ICU-level care in the air, so we knew she’d be in capable hands during the short flight across the lake.”
“It was a great outcome,” says Dr. Weisman, who was waiting at the doors of the ED to receive the inbound patient. “She avoided a lengthy stay in the ICU and was discharged a couple of days later, returning home in much better health.
